Écrit par : Justin Stolzenberg, Vice President, Argyle

Verification is becoming a budget and performance issue, not just a step in eligibility. Over the next two years, states may be moving to verify more often, with higher accuracy, and at higher volume, all while workforce capacity remains constrained. The result is a familiar pressure cooker. Agencies experience rising backlogs, more procedural denials, more churn, and greater exposure to financial penalties and corrective action plans.
Consent-based verification (CBV) is one practical way to reduce these risks.
CBV allows clients to authorize the agency to retrieve income and employment information directly from payroll and employer platforms—so eligibility decisions are faster, more accurate, and less dependent on paper documents.
The Verification Challenge: Where Traditional Methods Fall Short
States now face stricter accuracy expectations across benefit programs, and verification can be an important part of that. For the Supplemental Nutrition Assistance Program (SNAP), Payment Error Rates (PERs) above 6% will trigger additional financial penalties starting October 2027 in the form of a new benefit cost-share structure.
In addition, the effects of work requirements across SNAP, Medicaid, and the Temporary Assistance for Needy Families (TANF) program demand granular verification of income or hours worked for millions of enrollees. This can create a significant operational drag (such as cross-program case inconsistencies) on SNAP PERs.
Traditional verification methods create significant barriers:
- Manual processes can be slow and error prone. Caseworkers spend hours chasing documents, reconciling conflicting information across data sources, and entering data into multiple systems. Each step introduces the potential for delay and mistakes.
- In practice, verification bottlenecks show up as pending queues, repeat requests for information, more client contacts and complaints, and added supervisor review—all while agencies work to meet timeliness standards and prevent avoidable churn at renewal. These operational impacts—not the technology—are what drive higher cost per case and weaker performance outcomes.
- Legacy databases can be expensive and don’t often deliver visibility on income from the growing gig economy. As a result, many workers living with low-income—precisely the population agencies need to verify—don’t appear in these databases at all.
- Document-based verification creates an undue burden for applicants who are forced to locate, download, or request documents, then physically deliver or upload them. For those without reliable transportation, digital proficiency, traditional employment, or predictable work schedules, these requirements can prove insurmountable.
According to the Center on Budget and Policy Priorities (CBPP), the severity of coverage losses due to verification requirements “will depend not only on states’ policy choices, but their implementation choices as well.” CBPP research shows that eligible individuals lose coverage when they don’t understand what to report or how to report it.
Another major factor in coverage loss? When benefit administrators can’t verify submitted information accurately or in a timely manner. CBPP warns that hefty verification burdens could cause benefit administrators to fall behind on processing applications and renewals, threatening program integrity.
The Consent-Based Verification Solution
CBV transforms eligibility determination by connecting agencies directly to the source of truth: applicants’ actual payroll accounts. Through secure, consumer-permissioned connections, agencies access real-time income and employment data without requiring applicants to hunt down documents or caseworkers to chase information.
What CBV changes for agencies
The changes that CBV can achieve include:
- Fewer pending cases because verification happens during the workflow, not days later;
- Fewer client touchpoints (less mail, fewer uploads, fewer calls);
- Lower PER exposure through more consistent, direct-source verification; and
- More stable coverage by reducing documentation-related churn, especially at renewal.
Automated and Efficient
When an applicant connects their payroll account through a secure interface, complete income and employment data flows directly to the agency, eliminating the need for expensive reports, calls to employers, paystub collections, and data entry.
Argyle has run CBV pilots through the Centers for Medicare & Medicaid Services (CMS) and other partners, and are seeing dramatic efficiency gains:
- 31.6% reduction in decision time from application to eligibility determination
- 66% reduction in days pending post-interview as verification happens in minutes rather than weeks
- 93% of caseworkers find CBV solutions easy or easier to use than legacy methods
These reductions typically translate into improved timeliness, lower call volume, fewer escalations, and less overtime—while helping agencies stay ahead of accuracy expectations.
This efficiency doesn’t just benefit agencies—it directly reduces coverage losses. As CBPP emphasizes, states can mitigate harm by “maximizing the use of data sources to verify compliance and exemptions.” When verification happens automatically through consent-based, direct-source connections rather than relying on applicants to submit documentation, fewer eligible individuals fall through the cracks due to administrative barriers.
Dramatically Lower Costs

With a CBV provider like Argyle, state agencies can save up to 90% on verification costs compared to legacy databases and manual processes. These savings come from multiple sources, including fewer reverification charges, lower administrative costs, and improved accuracy. And with federal administrative funding declining, these cost savings become critical to maintaining operations without degrading service quality.
Superior Coverage
Adults living with low-income are significantly more likely to work in the gig economy, sometimes across multiple platforms. But traditional verification approaches often don’t capture gig income at all.
CBV solves this by connecting directly to gig platforms and capturing shift-level data. If an applicant works 15 hours driving for a rideshare, 20 hours delivering food, and 30 hours in retail, CBV automatically aggregates this information. Caseworkers see total hours worked across all sources, without applicants having to manually document every shift.
Enhanced Fraud Protection
Direct-source data is exponentially harder to falsify than paper documents. When income information flows directly from an applicant’s payroll account, agencies can be confident they’re seeing accurate, current information rather than potentially altered documents.
CBV detects fraud that traditional methods miss:
- Fake paystubs become ineffective when verification is provided by actual payroll systems.
- Misreported income is immediately apparent when direct-source data contradicts attestations.
- Superior coverage reveals total earnings that might not appear in traditional databases.
This enhanced fraud detection protects program integrity while ensuring that limited resources reach those who truly qualify for assistance.
Frictionless Applicant Experience
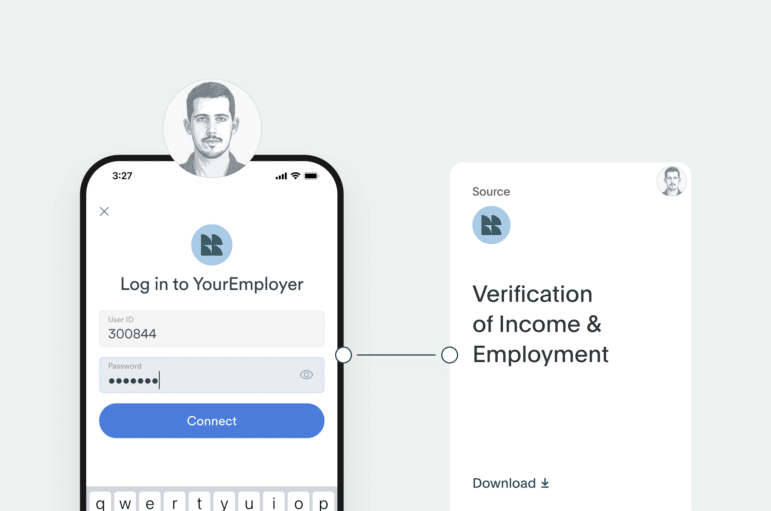
From the applicant’s perspective, CBV transforms what has traditionally been one of the most burdensome parts of the benefits application process. Instead of tracking down paystubs from multiple jobs, requesting employer letters, and waiting days or weeks for verifications to be processed, CBV allows applicants to authorize data sharing by simply signing in to their payroll account via a secure link.
Not only does this require less time and effort from applicants, it mitigates the confusion, worry, and delays they might experience during a traditional verification process due to uploading incorrect documentation.
Data shows that 85% of applicants report no difficulty verifying income through its consent-based platform, with a median completion time of just 6.7 minutes. And when applicants can quickly and easily verify compliance with work requirements or income limits, coverage losses due to administrative burden decrease significantly.
Protecting Applicant Privacy
Traditional verification creates unnecessary privacy risks. Paper documents containing sensitive information pass through multiple hands and systems, creating potential exposure points for data misuse or breaches.
CBV minimizes these risks through:
- Direct-source connections: Data flows directly from the source to the agency, bypassing the vulnerabilities inherent in manual document handling or intermediate databases.
- Explicit consent and control: Applicants authorize specific data sharing for a specific purpose, maintaining visibility and control over their information throughout the process.
For agencies, this approach supports privacy-by-design: minimizing data collection, limiting use to a defined eligibility purpose, and reducing manual handling of sensitive documents. This approach also builds trust with applicants while aligning with core privacy principles like minimizing data access. When applicants understand their data is protected and used solely for its intended purpose, they’re more likely to complete applications and maintain ongoing program compliance.
Verification Systems That Serve Everyone
Verification shouldn’t be the reason eligible families lose support—or the reason agencies absorb avoidable financial risk. As accuracy expectations rise and verification becomes more frequent, states can protect both access and integrity by reducing reliance on paper, fragmented data sources, and manual follow-up. Critically, it also creates an applicant experience that minimizes the administrative barriers that can cause eligible individuals to lose coverage.
CBV is one practical, near-term step: it strengthens verification where it matters most—income and employment—while reducing administrative burden for staff and clients alike. State agencies that implement CBV position themselves to meet today’s requirements while building capacity for tomorrow’s challenges. More importantly, they ensure that verification becomes an enabler of benefits access rather than a barrier.
L’objectif de Share Our Strength n’est pas seulement d’écouter les personnes touchées par ces systèmes, mais aussi de construire avec elles des systèmes plus performants. Le Conseil consultatif des parents et des aidants du programme SNAP veille à ce que ceux qui connaissent le mieux ces systèmes contribuent à définir ce qu’ils peuvent et devraient être. Leurs points de vue ont déjà influencé nos stratégies internes et nous aident à orienter nos priorités de programme vers des solutions plus efficaces.
À propos de l'auteur

Vice President at Argyle
Partagez cet article sur vos comptes de réseaux sociaux: